I began my professional journey as a practicing licensed therapist before transitioning into the mental health-related software development field. I’m now employed as a developer at Spring Health, working on their electronic health records (EHR) platform. My clinical background deeply influences my approach to programming.
Having spent time as a therapist in clinical sessions and as a user of various electronic health records platforms as a provider, I’ve experienced their clunky nature and inefficiency firsthand.
This is unfortunate for providers and clients because integrating a measurement-based care (MBC) approach in mental healthcare has the potential to improve client outcomes. It can systematically collect and evaluate client data and then use it to inform their care.
Mental healthcare providers could use an EHR platform that supports standardizing outcomes-based care in clinical practice.
MBC is essential for employers and health plans
Employers and health plans in search of an effective, comprehensive mental health support platform might consider the strategies employed by potential partners for implementing MBC into mental health treatment for their members.
Compass, Spring Health’s electronic health records platform, offers innovative features to assist providers in integrating MBC into their clinical practice. This integration improves outcomes for employees and health plan members and improves ROI.
Let’s explore how MBC can be used in mental healthcare, address its underutilization despite its proven effectiveness, and highlight how Compass is actively bridging this gap.
How does MBC work?
Throughout the history of mental health treatment, providers have operated under assumptions about the effectiveness of their treatment—which can, at worst, result in unintended harm to their clients. In other cases, they may be unable to gauge their treatments’ efficacy.
MBC includes evidence-based practices applicable to individual clients and broader population groups. At the individual level, this includes collecting data about client symptoms before, during, and after treatment to evaluate progress over the course of care.
On a larger scale, MBC extends to aggregating data for organizations, companies, or health plans seeking insights into population-level outcomes. This approach helps evaluate treatment effectiveness and offers valuable data for studying the impact of specific treatments.
Collecting data throughout care
Providers who embrace MBC regularly employ evidence-based assessments to check symptom acuity. This data becomes instrumental in adjusting the client’s treatment plan.
MBC places the individual and their symptoms at the center of the provider-client relationship, pivoting away from solely relying on the provider’s intuition to gauge progress.
Incorporating MBC into treatment equips providers with actionable data, offering a quantifiable measure of progress in mental healthcare. This is important for clients, providers, companies, and health plans seeking effective treatment outcomes for their employees or health plan populations.
MBC is underutilized
Research has shown that MBC improves client outcomes. However, its adoption within mental healthcare settings remains limited, with only about 20% of providers using it in their clinical practice. What contributes to this gap?
As a former therapist, I understand providers’ time constraints between sessions, often having only a few minutes to catch their breath. The added burden of sifting through assessments or searching for essential information while feeling rushed can create friction for providers.
Several barriers further hinder the integration of MBC into clinical practice:
- Poor EHR design: MBC dashboards are often separate from the EHR, making them easy to ignore and disconnected from the clinical documentation workflow.
- Additional provider burden: Implementing MBC often involves extra steps that disrupt the provider’s workflow, consuming precious time they may not have to spare.
- Non-actionable data: Assessment results are often presented in a format that lacks clarity, making it challenging for providers to quickly understand and implement them.
- Low clinician confidence: To actively embrace MBC, clinicians must grasp its value. Growing evidence shows that improved tooling alone does not improve MBC usage.
A noticeable disparity exists between our knowledge of MBC’s efficacy and seamless integration into the provider’s daily routine. Closing this gap remains a pressing challenge.
Compass bridges the gap
With Compass, our objective is to simplify the lives of providers while facilitating the standardization of outcomes-based care within their clinical practice.
At Spring Health, we’ve always utilized measurements as part of the care approach. When individuals seek care, they complete a series of clinically-validated assessments, giving the provider insights into their symptom acuity and establishing a measurement baseline.
Despite our longstanding use of measurements in care, we’ve noticed that providers don’t frequently consult the section within Compass where client measurements are stored.
Making MBC work for providers
Ideally, a provider would have access to the most recent assessment of client symptoms before a therapy session, enabling them to tailor their approach accordingly. To facilitate this, we’ve dedicated time to strategically place these measurements within the clinician’s workflow, ensuring they’re readily accessible.
Our goal is to integrate MBC into existing provider practices, making it faster and more convenient to use and encouraging increased adoption.
However, better tools are only one part of our four-pronged approach to standardizing the effective use of outcomes-based care. Our approach encompasses four key components:
- Simplified workflows
- Improved data visualizations
- Accessible education and change management
- Enhanced monitoring
Simplified workflows
Our Precision Mental Health assessment results are now integrated into clinical documentation on Compass. This integration will expedite decision-making processes and reduce the time required to access relevant data.
For example, following a therapy session, providers will receive a notification within Compass informing them of the duration since the client last completed an assessment.
With a simple press of a button within that notification, providers can send a reminder directly to the client, prompting them to complete the assessment. This approach eliminates the need for providers to manually track assessment timelines, locate the relevant tab, and initiate reminders.
Data visualizations
In our ongoing efforts to support providers, we’re committed to simplifying the process of visualizing a client’s assessment results over time. Traditionally, providers would review assessment scores individually, comparing results one assessment at a time.
We’re introducing enhanced charts with industry-leading design principles to streamline the workflow. These visual aids enable clinicians to visualize clients’ assessments throughout their care journey.
This enhancement is designed to eliminate the need for providers to engage in the time-consuming task of manually comparing scores. Instead, they can rely on one graph representing the client’s assessment results.
Provider education
Recognizing the complexity of Compass and the integration of MBC, we understand that expecting providers to navigate this on their own is a significant request. To support their journey, we offer a comprehensive package of resources.
This includes live and on-demand clinician-led training to provide insights into Compass and guidance on incorporating MBC into treatment. Compass also features prompts and explanations to facilitate use, complete with real-world examples representing the application of MBC during client care.
Additionally, Compass offers features such as hover-over explanations for specific tabs, providing information about their purpose. For example, providers can access details about the client’s medications, their intended purpose, and the prescribed dosage within the medications section.
Compass equips providers with the tools to utilize assessments and their resulting measures, empowering them to understand and integrate these insights into the client’s treatment plan.
Enhanced monitoring
Lasting behavior change among providers is monitored through Candela, Spring Health’s pay-for-performance system built on mental health outcomes. Candela ensures that members consistently receive high-quality care while supporting the professional growth of providers through data-driven insights and coaching.
Providers who use Compass also have a direct line to our development team, enabling them to report any issues or share feedback regarding what aspects of their workflow are beneficial and what may require improvement.
Integrating MBC is not solely about enhancing client outcomes and streamlining care. It's also about ensuring provider satisfaction. Spring Health has a 97% year-over-year provider retention rate. For MBC to truly become a standard in clinical practices, it must improve the lives of providers rather than add difficulty to their workload.
Additional features
Compass is a centralized hub where providers can access all relevant client medical information, including assessments, medications, and notes. Furthermore, it streamlines communication with other providers involved in the client’s care when necessary.
Among its additional features, Compass offers:
- Faster decision support: Real-time data and conversation prompts empower clinicians to prepare for sessions more efficiently, enhancing the quality of care.
- Compass data: Providers can leverage Compass data to identify clients who could benefit from other mental health tools, such as our Moments app, a digital resource library of mental wellness exercises and tools.
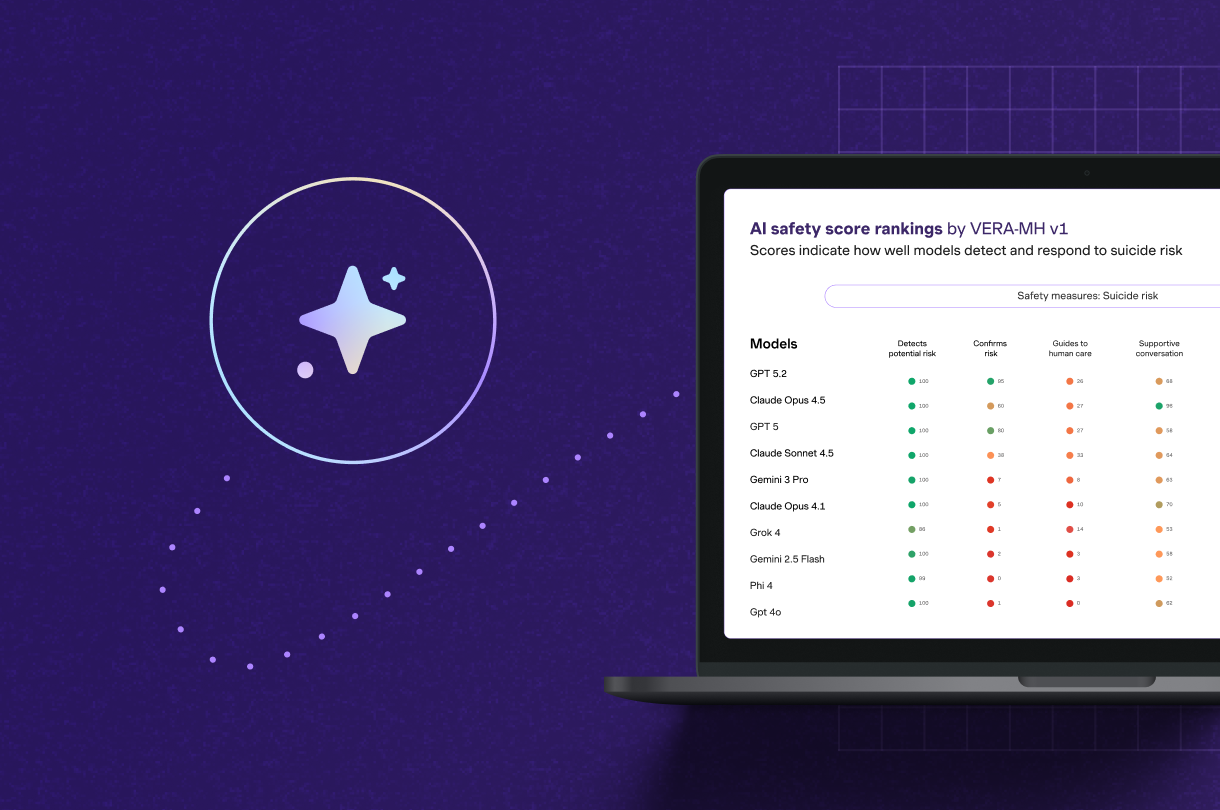
- Clinical safety: Compass prioritizes client safety by enabling providers to quickly evaluate positive screens for high acuity results, including suicidal ideation and self-harm. Pop-up alerts immediately notify the provider if the client has mentioned thoughts of self-harm or harm to others to any member of their care team.
- Information sharing: Compass facilitates information sharing between providers in one central location. This ensures a coordinated and comprehensive approach to client care.
MBC works. It’s time to make it standard in mental healthcare.
Measurement-based care is proven to be effective. However, a significant gap exists between this knowledge and the practical tools, education, and strategies required for providers to apply it effectively.
Compass bridges that gap by integrating measurement-based care seamlessly into provider workflows, offering at-a-glance data visualizations that reveal client trends over time.
Get your copy of our latest white paper for a deep dive into another key to modernizing mental healthcare—building better provider networks.

.jpg)
.jpg)

.png)
.png)


.png)